Normal Development of the Legs and Knees
Normal Development of the Legs and Knees
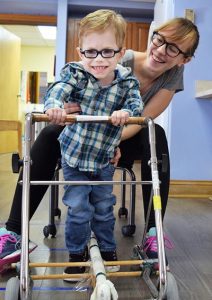
As children grow from toddlers to teenagers, normal alignment changes occur in their legs, so they may appear to be “knock kneed” or “bowlegged.” These changes may be of some concern to parents, who may then seek a professional opinion from a pediatric orthopedist. However, most children’s lower extremities follow a predictable pattern.
Bowlegs to Knock Knees
Bowlegs to Knock Knees
Most children are naturally bowlegged when they start to walk. Usually by the age of 2-3 years, the legs start to look more like knock knees. The knock knee phase peaks in the next 1-2 years. After six years of age the knees will normally assume a straighter alignment and there should be very little change in the angular growth. By 12 they have grown into what will be their adult configuration.
When a child’s angular profile (the angle of the thigh bone to the shin bone) or torsional profile (the knee and/or foot pointing straight, inward or outward) falls outside of the normal pattern, or if there is an abnormal profile only on one side (rather than bilateral), further evaluation is sometimes necessary.
Treating Deformity
Treating Deformity
If the angulation is extreme or asymmetric (only on one-side), further medical testing or consultation may be required. Medical treatment may be necessary to treat an underlying cause of angular deformities for conditions, such as rickets (which is caused by a vitamin D deficiency). Sometimes bracing or surgery is necessary, particularly for conditions such as Blount disease or growth plate injuries.
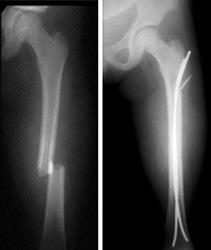
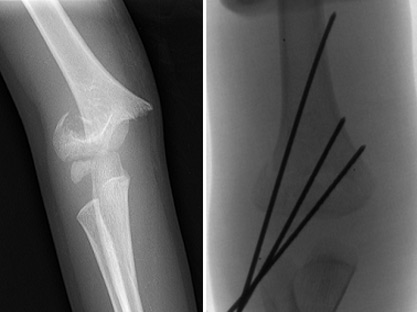
Damage to the child’s growth plate around the knee (the area of the bone where growth occurs in children) from fracture, injury, or infection can lead to unilateral varus (bowing) or valgus (knock knee). Although 15% to 30% of all childhood fractures affect the growth plate, serious problems due to growth plate injuries are fairly rare – consisting of 1% to 10% of all growth plate injuries - but are of concern nonetheless.
If the deformity is mild, it can be observed and carefully watched with x-rays and pediatric orthopedic exams over time. Surgical treatment may be required if the deformity becomes more pronounced. The type of surgery depends on the nature of the deformity as well as the age of the child.
Limb Lengthening for the Pediatric patient
Limb Lengthening for the Pediatric patient
Children who are born with—or who develop—differences in the length of their limbs can benefit from a range of treatments that may be as simple as the use of adaptive footwear or as sophisticated as limb lengthening surgical intervention that helps generate new bone in the affected limb. When limb lengthening surgery is indicated, orthopedic surgeons can safely and gradually lengthen the affected bone by up to 15 to 20 centimeters.
Although upper extremity bones such as the humerus (the bone that connects the elbow and shoulder joints) may be affected, limb length disparity is more typical in the lower extremity, particularly in the femur, the long bone in the leg extending from the hip to the knee joint.
Treating Limb Length Discrepancies
Treating Limb Length Discrepancies
Treatment decisions for patients with limb length discrepancies are based not only on the extent of the disparity at the time of diagnosis, but also on predicted increases in discrepancies over time. In order to make this prediction, the orthopedic surgeon takes into account the growth plate location, the age of the patient (i.e., the amount of growth remaining), and in the case of trauma or infection, the extent of injury to the growth plate.
In patients who have congenital limb anomalies of the leg, the predicted increase in limb length discrepancy can be calculated by comparing the short unaffected leg with the long unaffected leg; the percentage of growth arrest tends to remain constant during childhood. Use of growth charts in the equation help make the predictions more precise. In addition to these factors, the patient and family’s preferences and ability to follow up on needed care can play a role in treatment selection.
Our recommendations are made according to the following guidelines:
Our recommendations are made according to the following guidelines:
-
When the discrepancy between the limbs is small (less than two centimeters) use of a shoe lift is appropriate.
-
For those patients in whom the discrepancy ranges from 2-5 centimeters, a surgery called epiphysiodesis may be appropriate. This procedure slows the growth of the opposite leg or arm by altering the activity of the growth plate, thereby allowing the affected limb to “catch up” by the end of growth.
-
For discrepancies greater than three centimeters, however, limb lengthening may be an effective treatment choice.
Distraction osteogenesis describes the process of very gradual separation of the bone at the site of the incision and the formation of new bone tissue. Beginning approximately one week after surgery, the physician - and then later the parents and/or patient - adjust the fixator according to a precise schedule, usually three or four times per day. As the bone is distracted (or pulled apart), new bone forms at the gap as part of the healing process. The rate of distraction is very slow, with a standard increase of one millimeter (.0394 inches) per day.
PRECISE Tibia Animation
In pediatric patients, the orthopedic surgeon may use an external(Orthofix link) or internal(PRECISE link) lengthening device depending on whether there is other deformity to correct or not.
Depending on the planned lengthening, treatment typically continues for between 30 and 60 days. Following this stage of treatment, the frame remains on for an additional period of consolidation. This allows the regenerative bone to mature until it is capable of full, independent weight-bearing. When the surgeon has determined that this process is complete, the patient returns for removal of the frame or nail, a day surgery that is usually performed with the patient under sedation.
Limb Deformity conditions we treat:
Limb Deformity conditions we treat:
-
Bowed legs(Blounts disease)
-
Knock knees
-
Limb length discrepancy
-
Fracture malunions and nonunions and infections
-
Congenital limb deficiencies(fibular hemimelia, proximal femoral focal deficiency)